How to achieve good outcomes:
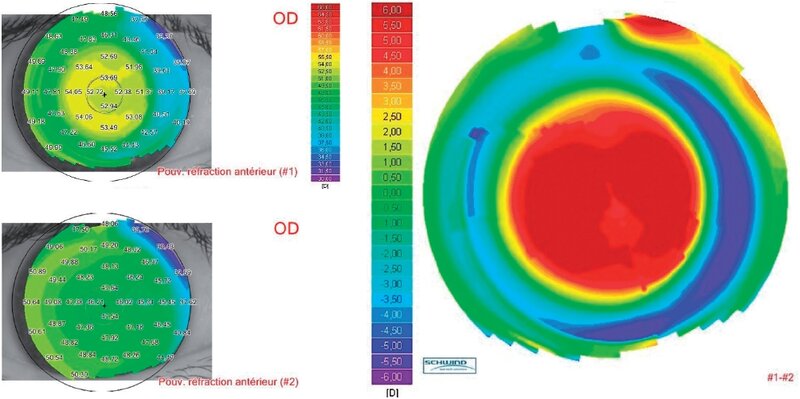
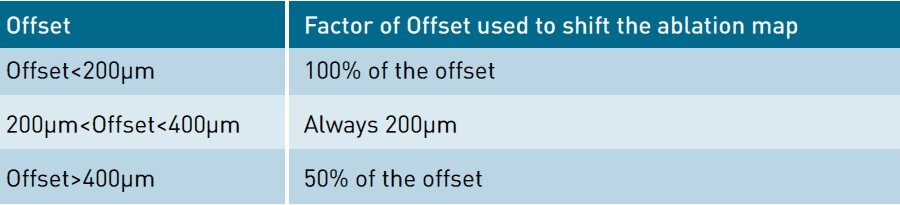
- Taking into account the often significant offset seen in high hyperopic patients, my technique is to shift the ablation map with the centration axis to minimize the induction of unwanted aberrations (figure 4).
- In a young farsighted patient it is common to see a big difference between the optical correction worn and the cycloplegic refraction. Wearing a higher optical correction for a few months may reduce the accommodative spasm and will allow a better correction of the true latent hyperopia.
- Small corneal limbal diameters may hamper the outcomes in high hyperopic treatments, since the cut may cause bleeding especially in contact lens wearers. These small corneal diameters are found most often in corneas with high hyperopia and steep keratometries. In those patients, the use of large treatment zones may be a contraindication.
- A discreet initial overcorrection is systematic both for hyperopia and for astigmatism. The patient should be informed about the visual discomfort in far vision during the early days of postoperative recovery.
Conclusion
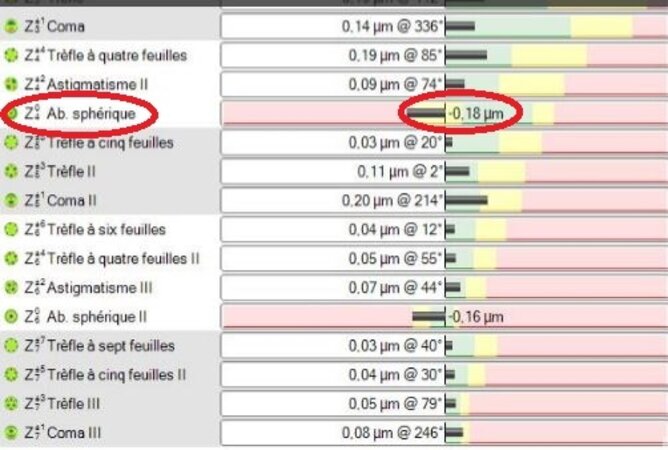
The bad reputation of high hyperopic corrections is linked to the deep ablations being performed in small optical zones and with a low optical quality, which may result in a high amount of aberrations. The consideration of centration axis and use of large treatment zones are the most important requirements for a successful outcome. The correction of high hyperopia is possible, however, following much stricter protocols compared to the myopic corrections. An imperfect realization of the intended hyperopic correction may have far greater consequences. But following these advices, and using modern technologies such as SCHWIND AMARIS, hyperopic corrections can be accomplished with greater level of success than ever before in LASIK up to +7.00D, whereas more concerns are associated with hyperopic corrections in PRK beyond +4.00D.